We have seen many health plans spend millions of dollars in HEDIS® analytics solutions and big data software, but left wondering what to do next! You can’t afford to ignore HEDIS® and Star ratings. Every incremental opportunity―whether small or large―needs to be squeezed to get to that all-important 4+ Star rating.
Payers with a 4+ Star rating receive 5 percent more county-based revenue from the Centers for Medicare & Medicaid Services (CMS) in addition to increased rebate percentages, which can be used to keep member premium costs down1. High Star ratings also offer a competitive advantage. In a 2018 report from Navigant, payers who improved from 3 to 4 Stars saw a 13-17 percent increase in member enrollment1.
Despite these incentives, Gorman Health Group reports only 45 percent of Medicare Advantage Prescription Drug plans (MA-PDs) earned 4+ Stars in 2019, just a slight increase compared to 44% percent in 20182―leaving plenty of room for improvement. Rather than increasing year over year, health plans saw a slight dip from 2018 to 2019 with their average Star rating (weighted by enrollment) moving down from 4.07 to 4.052.
Pairing up techno-functional subject-matter experts (SMEs) with data analytics investments should be part of your quality improvement strategy. Data analytics is both a science and an art and can involve some good-ole detective work!
Start by creating a team composed of experts with varied skills in areas like statistics, HEDIS® analytics, clinician analytics, R and SQL. Don’t overlook the importance of including someone with a strong client relationship background, as they can keep the attention focused on the results and not turn this into a R&D project.
Consider this your human data science team focused on identifying opportunities for HEDIS® and Star metrics improvement. HEDIS® measures and other evidence-based guidelines are grounded in an understanding of the human body.


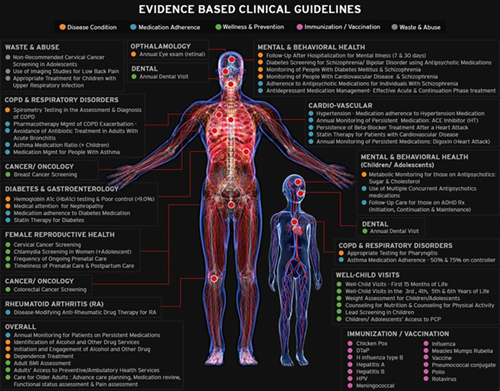
For example, a Medicaid plan’s rates for Antipsychotic Medication for Individuals with Schizophrenia3 dropped drastically after retrospective data refresh. The human data science team started by analyzing the entire process flow for this measure to uncover if there were any specific granular rules that triggered a drop of members.
A frequency distribution analysis of monthly Rx claims threw nothing out of the ordinary. A clinician conducting literature research realized that antipsychotic medications are “carved out” and must be billed to the state directly.
With this information the team went back to 10+ Rx data sources and were able to pinpoint a significant drop in data from one of their sources, resulting in members not crossing the 80% proportion of days covered (PDC) threshold.
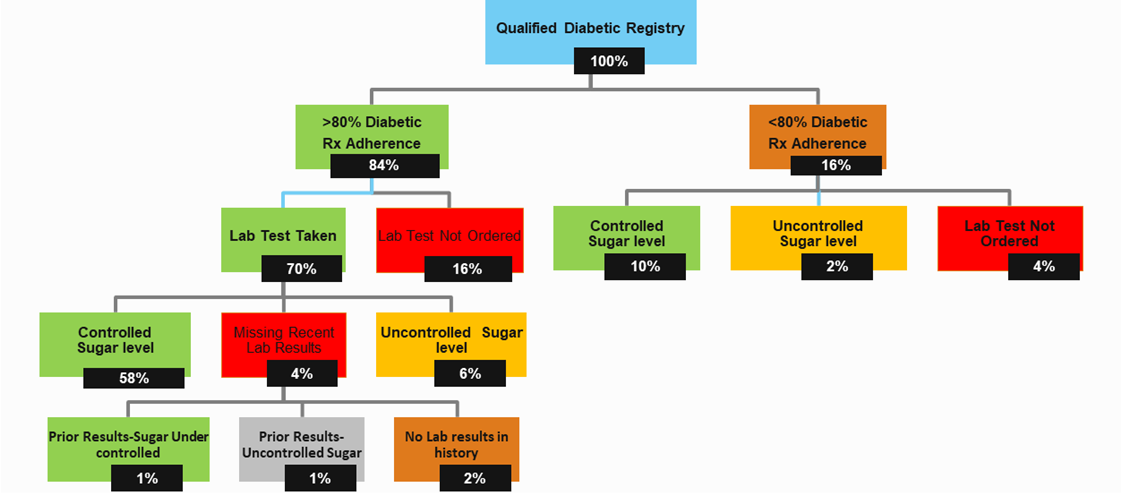
Another interesting analysis is a composite decision tree for the Star measure - HbA1c Control. Each node represents a cohort with potential unique barriers and opportunities. The team was able to determine that 24 percent of identified gaps existed due to a lab test that was not ordered by a physician or lab results gone missing from the completed order.
With benchmarks and thresholds continuously changing, payers need to approach their efforts as an ongoing and multi-pronged quality management improvement strategy. This means partnering with a proactive technology vendor who can go beyond the required HEDIS® measurement check boxes to help close gaps in care and improve quality ratings.
From Cognizant, TriZetto® ClaimSphere® is an end-to-end healthcare quality improvement solution that helps payers navigate the shift to value-based care. With 1 in 20 U.S. lives touched across Medicare, Medicaid and commercial LOBs, ClaimSphere clients have been able to achieve 4+ Star ratings, up to 45 percent increase in gap closures and receive Quality Bonus Payments from CMS.
Learn more about Cognizant’s digital solutions for quality management: www.cognizant.com/claimsphere.
HEDIS® is a registered trademark of the National Committee for Quality Assurance (NCQA). NCQA is a private, non-profit organization dedicated to improving healthcare quality.
- https://www.healthcarefinancenews.com/news/star-ratings-jump-strengthens-enrollment-performance-medicare-advantage-plans
- https://www.gormanhealthgroup.com/blog/the-2019-star-ratings-are-out/
- https://www.ncqa.org/hedis/measures/adherence-to-antipsychotic-medications-for-individuals-with-schizophrenia/
© 2019 Cognizant. All rights reserved.
Authors
Chenny Solaiyappan is a venture leader of TriZetto® ClaimSphere® QaaS at Cognizant and a Lean StartUp Practitioner with 20+ years of experience helping payers and providers with regulatory compliance and quality improvement initiatives. He is a self-trained data analytics and data science enthusiast offering thought leadership in the areas of healthcare quality improvement analytics.
Ritwick Goswami is a value-based healthcare SME with 10+ years of experience in HEDIS® and Star ratings and focusses on the roadmap for Cognizant’s quality improvement solutions. He leads the data analytics as a service team that delivers actionable insights to clients to improve their HEDIS® and Star ratings.
