WASHINGTON, D.C.—Don’t wait for lawmakers on Capitol Hill to solve problems related to health care. They aren’t going to do it, according to Rich McKeown, the keynote speaker at RISE’s National Summit on Social Determinants of Health. Instead of lawmakers, solutions will come from the 250 attendees of the conference who represent community-based agencies, health plan providers, service providers, and consultants who will drive necessary changes.
McKeown, chairman of the Leavitt Partners Board of Directors and co-founder of Leavitt Partners, emphasized the need for key stakeholders to collaborate to reach a consensus. “It’s the people who care about cost, care about quality, and care about patient engagement who are going to change the health care system.”
Jamo Rubin, M.D., president of Signify Community for Signify Health and chair of the conference, agreed that it will require cross-sector collaboration and the forming of alliances to move the needle on addressing social determinants of health. “We don’t have experience with this and it requires 350 million of us to do this work,” he said.

Collaboration hard at work
Health care organizations have slowly come to the realization that social, economic, and environment factors have a greater influence on a person’s health than medical care. Although many providers are in the early stages of establishing programs to tackle these challenges, one unique partnership that formed approximately four years ago shows that it is possible to work with multiple players in the community to improve the care of vulnerable populations.
Eric Epley, executive director of the Southwest Texas Regional Advisory Council, told attendees about the work of the Southwest Texas Crisis Collaboration. The group was formed in response to the growing number of people in the San Antonio area who were chronically ill, homeless, or had a mental illness, and who were frequently seek care in the emergency department and inpatient units. Indeed, 2015 studies revealed that there were 3,500 super users in the region who had more than 62,500 health care encounters in the health care system, equating to a cost of $175 million.
Part of the problem was the unnecessary emergency detentions of patients held against their will because they were a danger to themselves or others. An analysis of emergency detention patients on San Antonio emergency departments found that there were more than 9,000 emergency detentions each year, but half only needed a medical screening prior to psychiatric care. Instead, all these potential patients were sent to ERs and they became part of the national “boarding” problem, sometimes waiting 100 hours for care.


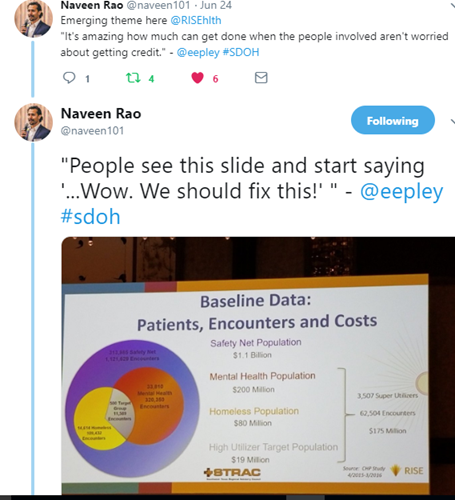
“The problem was the system we had wasn’t a system. It felt like a bunch of puzzle pieces in a Ziploc gallon bag, but we didn’t have the picture on the front of the box, and the front of the box is essential,” Epley said.
Competitors work together for the greater good
The group’s mission was to develop well-planned and coordinated regional emergency response systems and connect people who seek emergency services with the right type of care. The collaboration includes all major public payers, health system and hospital providers, philanthropy, public safety, the local mental health authority, behavioral health providers, and nonprofit organizations. A steering committee guides the work of the collaboration to ensure that members reach their overall goals: create a system of cross-sector providers, develop shared metrics, mobilize resources, and advance policy.
The key, he said, was the ability to work with engaged providers from the biggest health systems in the region. “It was all about collaboration, consensus and cooperation,” Epley said.
The collaboration created a 24/7 regional communication system that routes 500 trauma patients each month, coordinates air medical support, and has a computer aided dispatch system for all 911 calls related to mental health. All psychiatric facilities now actively use an online tool to notify the regional system of their diversion status and available beds are segmented by child, adolescent, adult, or geriatric. Patients are screened immediately so they can quickly get to the appropriate care setting.
“Trauma patients go to the trauma center. Stroke patients go to the stroke center. If a patient is medically stable we will take psych patients to the psych center, so they start getting care early and they aren’t sitting in an emergency department for hours,” he said.
The result: Patients receive the right care at the right time and place
In 2018, the system dealt with 16,138 cases. Epley said that 9,310 or 58 percent of the cases were sent directly to a psychiatric facility and 28 percent were sent to emergency departments. The patients were navigated to the right care, at the right time, and right place, he said.
The program is so effective that the collaboration is now working on additional projects, including the establishment of a 35-bed behavioral health diversion program. This program would provide 24-7 residential support with embedded outpatient treatment services, psychiatric emergency services to help facilitate transfers and care coordination to the most appropriate level of care, and the development of an intensive care coordination program to further reduce emergency detentions and the subsequent use of emergency and inpatient services.
